Understanding Sigmoid Colon Diverticulitis
Sigmoid Colon Diverticulitis develops when the diverticula, which are small pouches that line the wall of the sigmoid colon, become infected or inflamed. This problem manifests itself through a variety of unpleasant symptoms, including obvious stomach pain, bloating, fevers, and an inconsistent bowel movement pattern, which paint a picture of your lower digestive tract in distress. This region, located in the S-shaped section at the lower end of your large intestine, is particularly vulnerable to such problems due to morphological and functional differences.
Diverticula are very common, but when they get inflamed, that’s when diverticulitis turns from a silent spectator sport to an active participant one. This process highlights the need for medical intervention and highlights the delicate equilibrium found in our gut ecosystems. It also raises questions about the wider effects of lifestyle and dietary choices on our general health.
Many patients experiencing sigmoid colon pain may later discover that the underlying cause is sigmoid diverticulitis or sigmoid colon diverticulosis, especially when inflammation affects the lower left side of the abdomen.
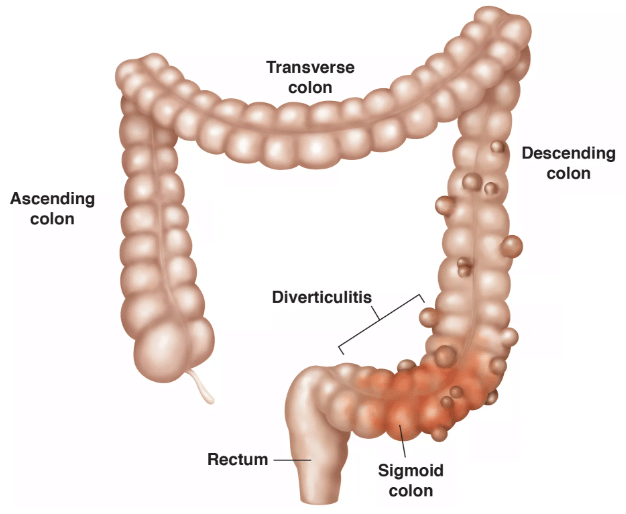
Understanding Sigmoid Colon Diverticulitis
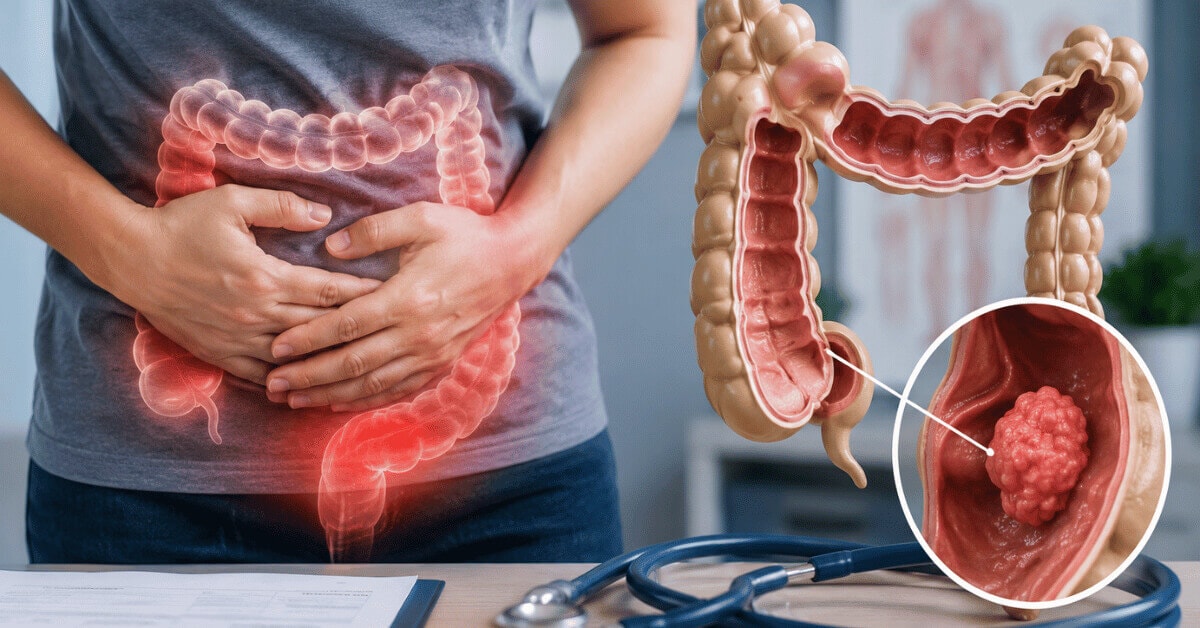
Diverticulitis is a disorder in which the digestive tract’s tiny, bulging pouches (diverticula) become inflamed or infected. These pouches usually occur in weak sections of the colon wall. Diverticulitis symptoms include abdominal pain (typically on the left side), fever, nausea, vomiting, changes in bowel habits, and, in some cases, rectal bleeding. It is frequently linked to a diet low in fiber and high in processed foods. Severe cases may necessitate medical intervention, such as antibiotics, pain medications, and, in some situations, surgery to remove the afflicted section of the colon.
The sigmoid colon Diverticulitis develops when the sigmoid colon’s tiny pouches (diverticula) become inflamed or infected. The sigmoid colon is the bottom section of the large intestine, right before the rectum. Diverticulitis normally develops when these pouches get clogged with debris, germs, or feces, resulting in irritation and, in rare cases, infection. In many cases, people diagnosed with sigmoid diverticulosis may not notice symptoms until the condition progresses into active inflammation or infection.
Diverticulosis vs. Diverticulitis: the Difference
Diverticulosis and diverticulitis are two stages on the colon health continuum that are frequently mistaken yet have separate characteristics. Diverticulosis is a disorder in which small, benign pouches, or diverticula, are present along the colon wall. For many people, this problem lives silently, without causing any discomfort or demanding medical attention. It’s like having unnoticed guests who don’t disturb the household’s calm. Diverticulitis, on the other hand, develops when these innocuous visitors become a nuisance, resulting in inflammation or infection of the diverticulum. This transition from calm to chaos is marked by a number of indicators that necessitate attention and management. The transition from diverticulosis to diverticulitis is an important stage in patient care, necessitating a sophisticated knowledge and treatment strategy. Recognizing this distinction is critical in navigating the route to appropriate care and relief from Diverticulitis-related symptoms.
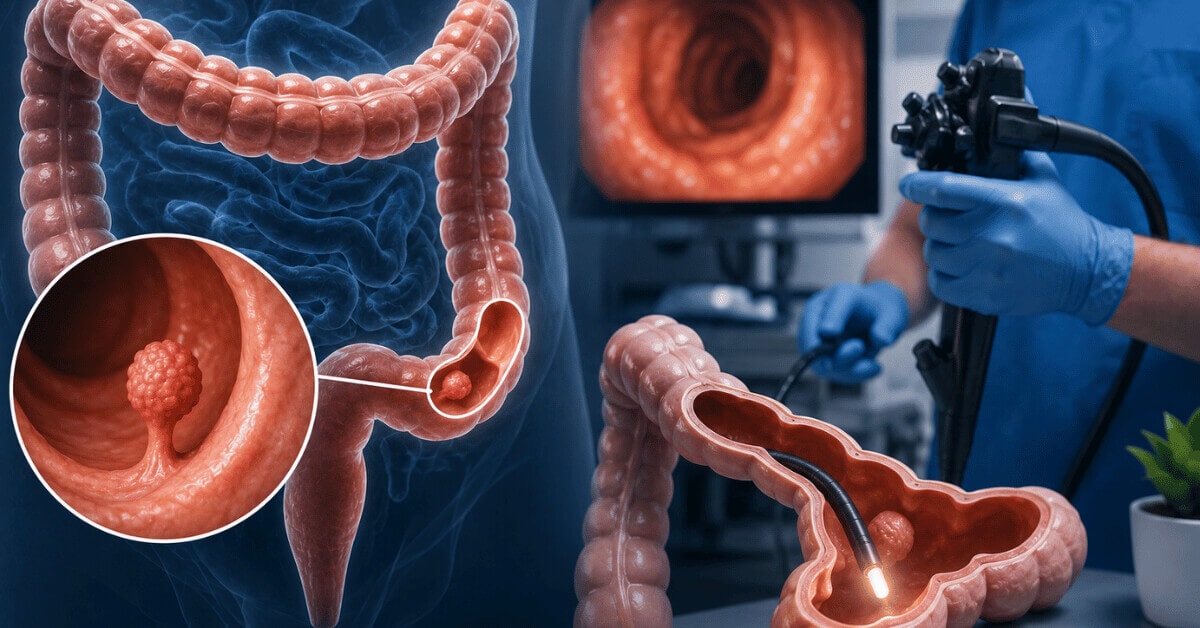
- Diverticulosis happens when small pouches or sacs, called diverticula, develop in the colon wall. It doesn’t typically cause symptoms and may go undetected until a person undergoes routine imaging tests or a procedure like a colonoscopy. This condition is commonly referred to as sigmoid colon diverticulosis when it affects the sigmoid portion of the colon.
- Diverticulitis occurs when diverticula become inflamed or infected. Diverticulitis typically causes sudden, severe abdominal symptoms, including persistent sigmoid colon pain, tenderness, bloating, and digestive discomfort.
The Path to Diverticulitis Treatment: From Diet to Medication
Taking the first steps toward controlling diverticulitis frequently requires a judicious combination of food changes and medication help. A fiber-rich diet is essential for this journey, allowing for smoother bowel movements and relieving strain on the colon’s walls, potentially preventing the beginning of future episodes. Antibiotics appear as a critical next step for patients dealing with illness, aimed at reducing inflammation and combating bacterial incursion. For those experiencing acute stages, switching to a liquid diet or introducing a period of bowel rest may be recommended, giving the digestive tract a much-needed break to promote healing. Engaging in this dual approach of dietary modification and medication underlines the proactive steps in addressing the symptoms and underlying causes of diverticulitis, setting the stage for a tailored treatment plan that resonates with the nuances of each patient’s condition.
Patients diagnosed with sigmoid diverticulitis are often advised to follow a high-fiber diet and maintain healthy digestive habits to reduce future flare-ups and manage symptoms effectively.
When is Surgery Necessary for Diverticulitis?
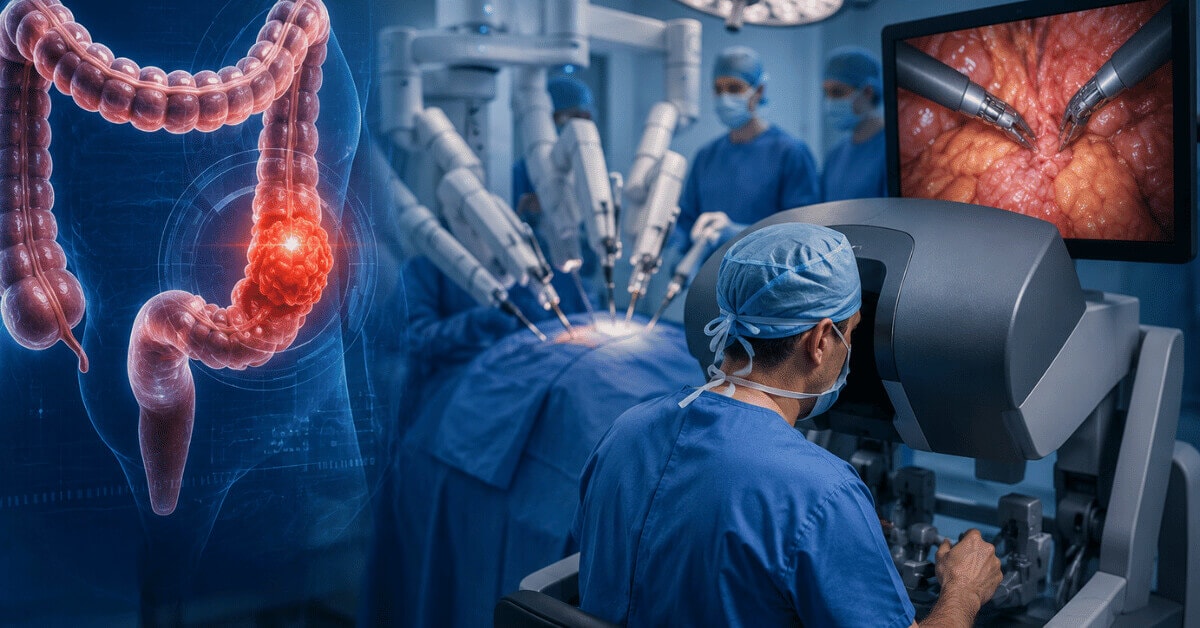
Surgical intervention for Diverticulitis, particularly of the sigmoid colon, becomes a conversation when conservative measures—dietary changes and medications—prove insufficient. It’s a pathway considered for those grappling with complications that risk the integrity of the colon, such as recurring inflammation, the formation of abscesses, or the emergence of fistulas. In instances where the disease lays siege to the body with relentless episodes or leads to significant structural concerns, removing the affected segment through a sigmoid colectomy may be the most viable strategy to restore health and stave off further distress. This step is deliberated in depth with healthcare professionals, weighing the potential for a substantial improvement in quality of life against the inherent risks surgery carries. This decisive move towards surgery underscores the severity of a patient’s condition and marks a pivotal point in their journey towards recovery, tailored to those for whom other treatments have fallen short.
What are the type of Surgery for Sigmoid Colon Diverticulitis?
- Bowel resection with primary anastomosis: In this treatment, your surgeon removes any contaminated colon (known as a colectomy) and stitches together the cut ends of the two healthy portions from either side of the previously infected area (anastomosis).
- Bowel resection with colostomy: In this operation, your surgeon conducts a colectomy and reconnect your bowel through an abdominal orifice (colostomy). This opening is known as a stoma. If your colon is extremely inflamed, your surgeon may perform a colostomy. Depending on how well you heal over the next few months, the colostomy might be temporary or permanent.
- Open: Your surgeon creates a six- to eight-inch incision in your belly to expose your intestinal tract.
- Laparoscopic surgery involves just minor incisions. The operation is performed by inserting small cameras and devices into your body via small tubes (trocars) that are typically less than one centimeter long.
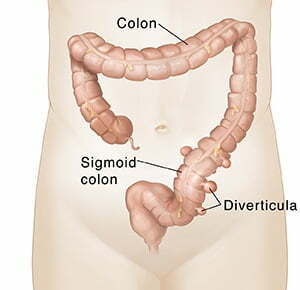
Is There a Cure for Diverticulitis?
Diverticulitis, a condition marked by the inflammation or infection of small pouches in the colon, presents a complex challenge in the realm of gastrointestinal health. It beckons a nuanced understanding that, although a definitive cure remains elusive, effective management strategies offer a beacon of hope. Embracing a multifaceted approach that marries dietary vigilance with regular physical activity forms the bedrock of staving off acute episodes and promoting long-term well-being. The emphasis on a fiber-rich diet underscores the pivotal role of nutrition in softening the impact on the colon, thereby reducing the likelihood of flare-ups. Regular engagement in physical activity complements dietary efforts, aiding in maintaining a balanced body weight and fostering optimal digestive function. The journey with diverticulitis is one of proactive adaptation and management, where the power lies in the hands of the individual and their commitment to a lifestyle aligned with intestinal health. Engaging closely with healthcare professionals to tailor a management plan that reflects personal health goals and challenges is essential, illuminating the path toward minimizing the impact of this condition on daily life.
People suffering from sigmoid colon diverticulosis should maintain regular medical checkups and dietary discipline to lower the risk of developing recurrent sigmoid diverticulitis attacks.
Navigating Life After Diverticulitis Surgery
Embarking on the recovery journey post-sigmoid Colon Diverticulitis surgery, it’s crucial to adhere to a prescribed post-operative regimen. This encompasses a meticulous approach to medication adherence, a phased reintroduction of solid foods, and steering clear of vigorous physical exertion during the initial healing phase. Adjusting to post-surgery life may present its set of challenges, including managing discomfort and adapting to new bowel habits. However, these are typically transient states that improve with time. Proactive participation in follow-up care is key—ensuring open communication with your healthcare team to effectively monitor your healing trajectory. With diligent post-surgery care, individuals can anticipate a return to their daily routines, empowered by an enhanced quality of life.
How long does it take to recover from the Diverticulitis surgery?
You’ll be in the hospital for two to seven days following this procedure while your physicians watch you and ensure you can pass waste again.
When you get home, do the following to help you recover:
- Do not exercise, carry anything heavy, or engage in sexual activity for at least two weeks after leaving the hospital.
- Avoid lifting since it can be life threatening after cure of diverticular disease.
- Depending on your preoperative state and the outcome of your operation, your doctor may suggest that you follow this limitation for a longer or shorter time.
- Begin with just clear beverages, eat high fiber food, lots of fiber diet, and healthy anti inflammatory food habits.
- Slowly reintroduce solid meals into your diet when your colon recovers or as instructed by your doctor.
- Follow whatever instructions you were given for caring for your stoma and colostomy bag.
If you have symptoms of sigmoid colon diverticulitis, you should seek medical assistance immediately since the illness can lead to problems such as abscess formation, colon perforation, or fistula formation if left untreated. Antibiotics are often used to treat the illness, followed by dietary changes and, in extreme situations, hospitalization. In certain cases, surgery may be required, particularly if complications arise or the problem recurs repeatedly.